06 Mar Diabetes and why you should see a podiatrist
Diabetes is a complex condition which can affect your entire body. There are three main types of diabetes; type 1 diabetes, type 2 diabetes and gestational diabetes. There is currently no cure for diabetes, but people who manage it well have a normal life expectancy.
Diabetes and the body
Having diabetes means that the body cannot maintain a normal level of glucose (sugar) in the blood. High amounts of glucose in the blood can lead to health complications.
For the body to function normally, it must convert the glucose into energy for the body to use. Insulin, a hormone, is ‘the key’ that converts glucose into energy. People with diabetes do not produce enough insulin (or produce none at all) to convert glucose into energy. When they eat foods such as bread, pasta, fruit, milk and sweets the sugar from these foods (glucose) cannot be converted into energy for the body to use. Instead it accumulates in the blood causing high blood glucose (sugar) levels.
 Diabetes and the feet
Diabetes and the feet
Uncontrolled blood glucose levels can cause hardening/narrowing of the vessels down to the feet, and honey-like blood flow. The cells of the feet are eventually starved of nutrients and energy. The feet become unhealthy (dry skin, poor nail quality and decrease muscle integrity) and the nerves die leading to neuropathy (sensation loss). The overall lack of sensation means that regular knocks, bumps, bruises, scratches and cuts will not be detected and the lack of blood supply means that these areas won’t heal properly and may become ulcerated. Ulcers are entry points for nasty infections. If an infection is bad enough, amputation of the unhealed, ulcerated and infected site is the only solution.
Avoiding foot-related complications
Risks such as neuropathy (sensation loss), ulceration and amputation can be reduced with regular foot checks by a podiatrist and by talking good care of your feet at home and checking for any changes daily.
What is a foot check?
A foot check by a podiatrist looks at the condition of the feet; the shape, the skin and the toenails. Any current problems are assessed and/or they decide how likely a person with diabetes will develop future foot-related complications.
A podiatrist will:
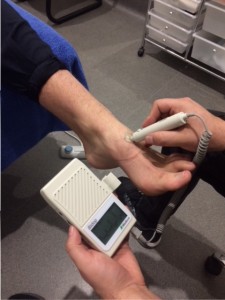
- Check the pulses in the feet to assess the quality of blood flow.
- Check the nerves in the feet (touch and vibration) by using piece of fishing line (monofilament) and a tuning fork.
- Check your shoes and overall fit.
The risk categories
LOW RISK
- If pulses are present with good quality blood flow.
- NO nerve damage.
- NO changes in the shape, skin or toenails.
HIGH RISK
- If pulses are NOT present.
- Nerve damage and sensation loss (neuropathy).
- Changes in the shape, unhealthy dry, cracked callused skin or unhealthy fungal, thick or ingrowing toenails.
NOTE: Seek help urgently if there are signs of infection, skin break down, new pain, swelling or redness.
Podiatry management options
- Regular routine care to treat long, thick, mycotic toenails or hard skin (callus and corns).
- Footwear advice and referral for appropriate shoe fit, comfort and support.
- Orthotic therapy for pressure offloading and soft tissue assistance.
- Balance and strengthening exercises to do at home.
- Wound treatments; dressings, self-care, healing promotion and onwards referral.
- Self-care tips at home, like checking feet daily and washing/drying/applying moisturizer.
For more information on caring for your feet, check out:
Diabetes Australia 2018 https://www.diabetesaustralia.com.au/caring-for-your-feet


